
The text pinged my phone before 7 a.m. on a late November morning. I’m accustomed to these early messages from my friend Cynthia, a staunch early riser. Usually the texts relate to her guide dog and BFF, who enjoys a playdate once per week at a nearby dog boarding service. I serve as the sweet yellow Lab’s willing chauffeur.
But this text was different—longer than normal and shot with frustration. The day prior, Cynthia had received a letter from the Montana Department of Health & Human Services (DPHHS) informing her that her Medicaid redetermination deadline was just a week away. Cynthia had been on Medicaid since 1991, and as a veteran of the low-income medical insurance program, she was intimately familiar with the annual process in which recipients submit information to the state to confirm their continued eligibility.
The problem with this letter?
It was the very first communication about the imminent deadline that she had received. And that meant she had little time to fill out the paperwork and submit it before she was kicked off Medicaid and left without coverage.
Cynthia is completely blind and deals with several serious medical conditions that cause her significant chronic pain. Still, for more than 30 years, she had sailed through the Medicaid redetermination process. In years past, she would receive the next redetermination date when her application for the current year was approved. Typically, that means she has a year’s notice. Paperwork would arrive at the beginning of the month prior to the redetermination date, giving her two months to complete and submit the paperwork. Redetermination has been, for obvious reasons, hugely important to her well-being. It was always completed with plenty of time to spare, and she had never come close to missing a deadline.
Despite physical limitations that would conquer even the toughest among us, Cynthia maintains a stoic demeanor, a wry sense of humor, and a genuine generosity of spirit. She’s also smart as a whip, fiercely independent, and stubborn as hell. So when she asked for help on that November morning, it was clear she was in a bad spot.
Would I be able to help?
“If I’d received this crap last month, I wouldn’t be asking…,” she wrote in the message.
She had already spent several fruitless hours on hold with DPHHS the previous day, and the assistive technology on her phone and computer that enables internet navigation had proven no match for the agency’s woefully overburdened website.
Despite physical limitations that would conquer even the toughest among us, Cynthia is fiercely independent and stubborn as hell. So when she asked for help on that November morning, it was clear she was in a bad spot.
As we would soon discover, Cynthia was not the only person dealing with redetermination snags. Far from it. Montana’s Medicaid “unwinding” process has been a bureaucratic debacle that’s even left those who’ve been able to keep their Medicaid coverage tied up in knots.
So, how did we get to this point? Medicaid is jointly funded by the federal government and the states. The share of federal funding varies from state to state because the program is designed to provide more help to states with lower per-capita incomes. The latest data from the Kaiser Family Foundation—an organization dedicated to health policy research and reporting—indicates that in Montana the feds cover roughly 65 percent of the Medicaid tab, with the state picking up the remainder. Each state is also responsible for managing Medicaid eligibility and distribution.
When the Covid pandemic hit, the federal government put a moratorium on redeterminations, meaning that every person who was on Medicaid continued to receive those benefits, and every new recipient who qualified was also automatically renewed. When the Biden administration officially ended the pandemic-related public health emergency early last year, that moratorium also ended.
For the first time in three years, states were back in charge of managing, or “unwinding,” their Medicaid redetermination processes. The vast majority of the estimated 90 million Americans receiving Medicaid benefits in 2022 would be evaluated for continued coverage. Some people would no longer qualify due to things like changes in income and some people would not reapply for a variety of reasons. So it was no secret the moratorium’s end would result in people losing benefits. KFF estimated that more than 20 percent of Medicaid recipients in Montana (around 60,000 of the roughly 280,000 enrolled) would lose coverage—a potentially significant blow to the affected individuals and families, as well as to the health care services that support them.
As it turns out, KFF’s estimate vastly undershot Montana’s actual disenrollment rate. The latest data from Montana’s redetermination dashboard indicates that nearly 133,000 of the state’s Medicaid recipients have lost coverage. That equates to an overall disenrollment rate of 55 percent, which is higher than every state except Utah, according to KFF’s Medicaid Enrollment and Unwinding Tracker.
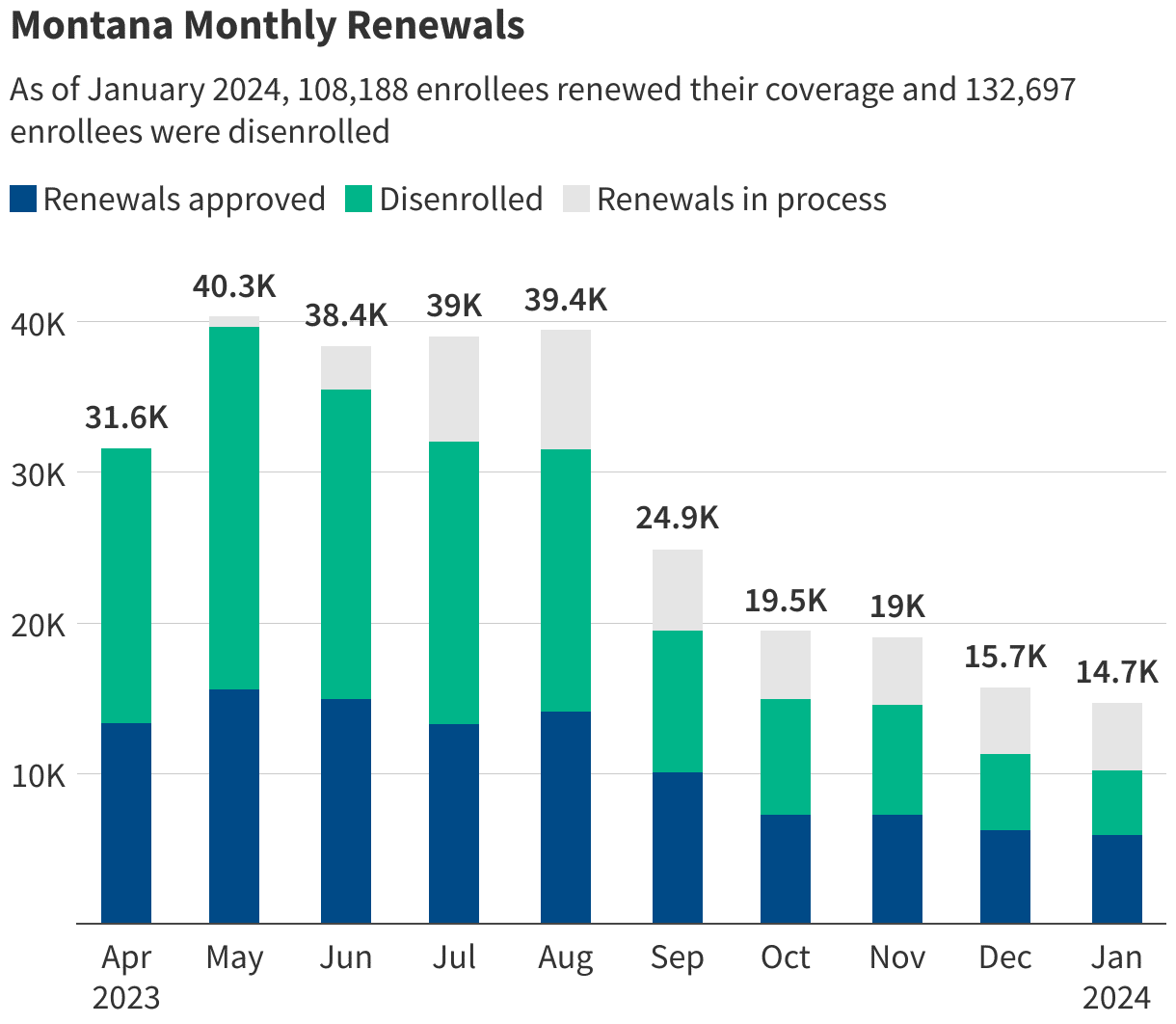
Of those 133,000 Montanans, 64 percent (about 85,000 people) lost Medicaid coverage due to applicants’ “failure to provide requested information,” while only 30 percent (about 40,000 people) were actually deemed ineligible.
KFF includes that 64 percent in a category it calls procedural disenrollments.
“High procedural disenrollment rates are concerning,” KFF notes on its website, “because many people who are disenrolled for these paperwork reasons may still be eligible for Medicaid coverage.”
The reasons for the high disenrollment rate remain unclear. There have been plenty of anecdotal complaints about long wait times on the phone, staff shortages, and website issues, but DPHHS has offered little in the way of explanation. Cynthia’s situation suggests paperwork snafus have affected qualified people’s ability to maintain coverage, and in her case, at least, those aforementioned issues compounded the problem.
The state has defended its handling of Medicaid redetermination even as health officials at the federal level express alarm over the number of Montana children left without coverage, and as the strain of redetermination leads to “unacceptable” delays in processing SNAP applications. The agency has acknowledged that it’s “strapped,” and it’s also pinned some of the blame on applicants being slow to return their paperwork.
Last week, Montana Democrats held a news conference at the State Capitol to highlight the people affected by unwinding. A spokesperson for Gov. Greg Gianforte’s office told KTVH News the event showed how “far-left activists … want to overburden the system by keeping folks who are ineligible on the rolls and having Montana taxpayers foot the bill.”
The redetermination dashboard states that “individuals who are required to return information will be mailed a redetermination packet, mailed and texted a reminder notice, and mailed a determination notice at least 10 days before loss of coverage.”
Cynthia, who does almost all of her shopping online and checks her mail daily, is certain she never received a redetermination packet. She says she didn’t get a reminder either, by mail or by text. The only notice she did receive was meant to serve as the final notice, eight days before her redetermination deadline.
It was a couple of days before I could help Cynthia in earnest. By then she estimated she had spent somewhere north of 10 hours waiting on the phone or unsuccessfully navigating the website. She still didn’t have the paperwork she needed—that elusive redetermination packet. At her behest, I logged into her DPHHS account to track them down. I could not locate those documents on the website, though admittedly I lost some enthusiasm for the search the third time I was kicked off the website and then logged back in to find no evidence of my progress the site had supposedly saved.
Having given up on the website, I spent much of the next few days on hold with DPHHS or waiting for a callback that never came. The person I finally connected with was not a DPHHS specialist, but a temp hired by the department in the wake of the federal government’s reprimand of Montana DPHHS over excessive wait times on the Medicaid hotline. She was kind and understanding but had no better luck than I did in tracking down Cynthia’s paperwork. She recommended that I go to the local Office of Public Assistance to get things figured out.
Missoula’s OPA is one of 19 such offices across the state that offer help to folks enrolled in any number of government assistance programs. I had heard horror stories of long lines and wait times at OPA, particularly in the mornings. But when I went there the afternoon before Cynthia’s deadline day, I got lucky. The line was short and it took less than 20 minutes to pick up her redetermination paperwork.
“High procedural disenrollment rates are concerning because many people who are disenrolled for these paperwork reasons may still be eligible for Medicaid coverage.”
As I was leaving, it suddenly occurred to me that I hadn’t received any notice from DPHHS about my 18-year-old son, who had been enrolled in Healthy Montana Kids, a Medicaid program that allows families making as much as 250 percent of the federal poverty line to access health insurance assistance for their children. It was overwhelmingly approved by Montana voters via ballot initiative in 2008.
I work multiple jobs and my wife owns and runs a small business, so for years it’s made sense for us to buy our health insurance through the Affordable Care Act marketplace, which automatically enrolled our son in the Healthy Montana Kids plan. As in previous years I had planned on renewing our policies in December, but figured I’d check with the folks at the OPA just in case. I’m glad I did, because I was informed that my son’s redetermination deadline was the same as Cynthia’s—the very next day. Like Cynthia, I had been on the lookout for any material from DPHHS. Unlike her, I didn’t receive even a single notice about my son’s case—no redetermination packet, no reminders of any sort, and no 10-day notice of termination. I had less than 24 hours to gather the necessary records and complete our redetermination paperwork. I told the woman at OPA about not receiving any notices, and she took note.
The following day—deadline day—I dropped off both sets of paperwork. A kind OPA staffer assured me Cynthia’s application was complete. Cynthia called DPHHS the following day to set up an interview. She knew to do that because before the Covid moratorium on redetermination, phone interviews were a mandatory part of the process. But this time, she was told that she “couldn’t wait until the last minute and expect things to be done just for [her],” she paraphrased, and to call back the following Monday.
Cynthia attributed the snide comment to the immense pressure the hotline folks had been under, since most of the people we had interacted with had been at least understanding, if not helpful. On Monday she was told that interviews were no longer needed, but that her paperwork was in order and that she would receive notice via mail if there were any changes to her Medicaid status.
Remember how I told the woman at OPA about not receiving my son’s Healthy Montana Kids paperwork or any notices? A couple weeks later, in mid-December, I got a letter in the mail. It was printed Dec. 13, but the letter itself was dated Oct. 6. It informed me that someone in our household had lost Medicaid or Healthy Montana Kids coverage because the redetermination packet—the one that never arrived (and I didn’t know to expect) in the first place—had not been returned.
There’s another factor to consider. KFF data indicates that after Biden lifted the moratorium on redetermination, 43 states chose to complete redetermination over a 12- to 14-month period. Montana chose to complete the review process on a more aggressive timeline—only 10 months. KFF notes that a number of states have responded to high initial disenrollment rates by pausing disenrollments while they address problems in the process.
In December, two members of the state legislature’s Health and Human Services Interim Budget Committee asked DPHHS Director Charlie Brereton to pause the process, citing concerns over the high disenrollment rate and continued reports of long hold times. Brereton declined the request.
For Cynthia, the month of December was a quiet one on the Medicaid redetermination front. With no further contact from DPHHS, Cynthia had seemingly satisfied the requirements after our all-hands-on-deck deadline week. But then, in the first week of January, I got a mid-afternoon call from her. I had dropped her pup at doggy daycare early that morning, so a call from her was unusual, since I would be seeing her when I brought him back later in the afternoon.
“You’re not gonna believe this,” she said.
She explained that when she checked her bank account to confirm the deposit of her modest Social Security check, she found that the money had evaporated the moment it reached her account. Montana DPHHS had closed her Medicaid case without re-enrolling her, and had done so without any notification. As a result, the Medicare premium that had been previously covered due to her Medicaid eligibility had been withdrawn from her bank. She was flat broke, with several bills coming due.
Could I get over to her mom’s house to pick up a check and get it to her bank?
I raced to her mom’s, got the check, and deposited it for her.
Cynthia called DPHHS early the next morning. An agent reviewed her case and found that it had simply “not been worked,” as Cynthia remembers him saying. In other words, Cynthia had done everything correctly but her application had apparently landed in paperwork purgatory and overlooked by the harried staff at DPHHS. Cynthia’s Medicaid account was reactivated within 24 hours, and not long after that she received a refund for her Medicare premium.
Still, Cynthia’s botched redetermination has her questioning the competence of the agency and its leadership. And while she averted crisis, the same can’t be said for all of the other 133,000 people—about one in 10 Montanans—who, for one reason or another, have been removed from Montana’s Medicaid rolls.
That’s a “pretty staggering coverage loss,” Olivia Riutta said last week in Missoula as the group she directs, Cover Montana, announced a new campaign to help people regain health care coverage as quickly as possible, as Montana Free Press reported.
Cover Montana is an arm of the Montana Primary Care Association, and its “Get Covered Again” campaign is working to ensure that the many newly uninsured Montanans don’t “join the long-term ranks of the uninsured,” as Riutta was quoted as saying.
To avoid those ranks, Cynthia has a plan.
“I can guarantee that I will be calling them in early October,” she says of her presumed 2024 redetermination window. “I can’t let them screw it up again.”
But this whole mess has left us both with a great deal of concern for those Medicaid recipients who, unlike Cynthia, are inexperienced in the system or didn’t have friends or family to help them navigate the process. How many of those Medicaid-eligible folks find themselves without health insurance right now? What happens to them?



